Innovative Education
There is evidence that past ALS training programmes have proven inconsistent and inadequate, with numerous studies reporting trainees have poor retention; and, therefore, ineffective ALS skills as a result. Most life support courses taught in Australasia, and across the world, are based on a similar model; comprising a print manual, with variable quality of text and illustrations, followed by a face-to-face course which includes a number of PowerPoint-based lectures, small group skills teaching, then practice and assessment based on low-level simulation scenario training.
Published evidence suggests that many of these elements are flawed, and result in less than ideal educational outcomes. Logically, if courses which train clinicians in the recognition and management of time-critical diseases, in particular cardiac arrest with its overall survival of under 10%, are not effective in achieving the educational outcomes they are supposed to, this may have an impact on patient outcomes, and even survival.
In 2018, the American Heart Association stated “The AHA believes that poor CPR quality is a preventable harm”.
“Educational Strategies to Improve Outcomes from Cardiac Arrest examines best practices in education and applies them to resuscitation science. When implemented in training, guidance in this resource will help raise quality of care and increase survival from cardiac arrest”.
Within the material in this AHA Education Statement was a quote from the Chair, AHA Scientific Statement Development Committee who said “If all training programs and resuscitation instructors implement the guidance from this statement, it will improve performance and increase survival from cardiac arrest.”
Among the recommendations made to revolutionise resuscitation training were…
Mastery Learning and Deliberate Practice
Knowledge Translation and Implementation
Contextual Learning
Spaced Learning
Mastery Learning
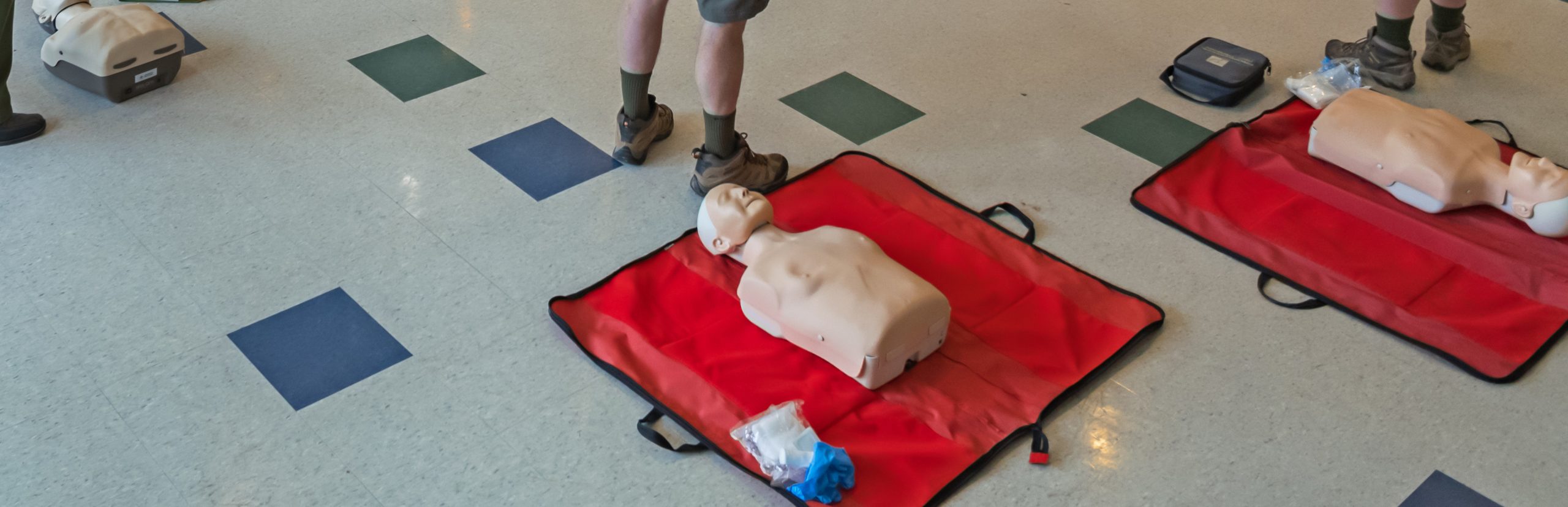

The ARLS course utilises mastery learning initially in teaching High-Quality CPR (HQ-CPR) where candidates are issued their own personalised mannequin and repeatedly perform supervised practice with feedback throughout the face-to-face skills day.
Performance is closely assessed and candidates take the mannequins home with a planned HQ-CPR performance revision program; they are also encouraged to teach family and friends as part of a program to increase bystander BLS in the community. Other incorporated mastery teaching includes bag-valve-mask ventilation and safe defibrillation.

The Practitioner Immediate Life Support (PILS) course primarily concentrates on the practical skills needed for the management of cardiac arrest, although the principles of systematic examination, in order to recognise the peri-arrest patient, are strongly emphasised. HQ-CPR skills are repeatedly practiced under supervision throughout the course.
The PILS course enables highest quality learning in a short, half-day course tailored for in-hospital clinician allocated training time, still benefitting from the innovative AICE video-based prelearning, and spaced-education post-learning knowledge consolidation and assessment.
Knowledge Translation and Implementation

The Education Statement says “Principles from knowledge translation and implementation science (i.e., applying evidence-based research in the clinical practice) should inform efforts at the local level.” The first principle is that we should enhance passive knowledge translation with active techniques.
A variety of efforts are being made to shift the curriculum of medical training from a teacher-centred to a learner-centred model. The ‘flipped classroom’ has been shown to be an effective teaching method for changing students from passive to active learners and creating integrative educational strategies, as class materials are provided ahead of time for students to study alone, while activities that require students’ active participation are the focus during face-to-face classes.
Studies have shown that emergency medicine students who learned about ALS in a flipped classroom versus those who had learned using lecture and simulation, showed that the flipped classroom students scored higher than the others. In 2020, the International Liaison Committee on Resuscitation stated that “…recommends providing learning formats as pre-course preparation for advanced courses…strongly recommends providing the option of e-learning as part of a blended learning approach.”

The ARLS course is based upon an innovative blended learning approach, which has been found to so successful in delivering knowledge in preparation for face-to-face advanced clinical skills courses. Candidates are given access to comprehensive pre-learning comprising a series of broadcast-quality, studio-recorded videos, incorporating the Recognition of Serious Illness (ROSI) modules, followed by a number of focused modules on Clinical Skills, patient assessment and the ALS algorithm.
The face-to-face ARLS course component comprises a single day, tightly focused and planned around mastery and contextual learning, also incorporating human factors training and discussion of challenging resuscitation decisions, with knowledge being consolidated and assessed by a novel spaced education series of questions, delivered over a period of weeks, as discussed below.

The PILS course is based upon an innovative blended learning approach, which has been found to so successful in delivering knowledge in preparation for face-to-face advanced clinical skills courses. Candidates are given access to comprehensive pre-learning comprising a series of broadcast-quality, studio-recorded videos, incorporating focused modules on Clinical Skills, patient assessment and the ALS algorithm.
The face-to-face PILS course component comprises a half-day, tightly focused and planned around mastery and contextual learning, with knowledge being consolidated and assessed by a novel spaced education series of questions delivered over a period of weeks, as discussed below.
Contextual Learning
A core concept for instructional design of resuscitation training is the applicability of training experiences to each learner’s real-world scope of practice. The AHA Educational Statement suggested that “…courses with content targeted to the learner warrant further exploration”, based on evidence that hospital-based providers achieved critical clinical tasks at a significantly higher rate during simulated cardiac arrest after training with learning objectives specific to in-hospital cardiac arrest management.
The Statement also says “Multiple studies have demonstrated that standardized team training as a supplement to BLS or ACLS courses can enhance team dynamics and communication and may contribute to improvement in technical skills” with one study demonstrating 2-fold increase in the odds of patient survival during actual in-hospital cardiac after specific team training.

The face-to-face ARLS course is taught by highly experienced and trained instructors from a variety of clinical backgrounds, including medicine, nursing and paramedicine, with some instructors having a background in more than one clinical domain.
Contextual learning is implemented in all training scenarios, with ARLS instructors bringing context and experience from every potential setting, and with understanding of every possible cardiac arrest team configuration, from remote and austere prehospital scenes to tertiary emergency medicine and intensive care.
Cognitive stress loading is carefully managed by innovations such as the use of recorded background noise levels, with specific human factors and non-technical skills teaching from experts from medicine and aviation.

Similar to ARLS, the PILS course is course is taught by highly experienced and trained instructors from a variety of clinical backgrounds, including medicine, nursing and paramedicine, with some instructors having a background in more than one clinical domain.
Contextual learning is implemented in all training scenarios, with the PILS course being delivered on-site at health facilities such as hospitals, GP surgeries and other settings.
Spaced Learning

The AHA statement states “Resuscitation training involves the acquisition of specific knowledge, skills (psychomotor, teamwork, communication), and attitudes with the goal of maximizing performance during patient care.”
Standard ALS courses are solely based around a 1-2 day face-to-face course, with a substantial component taken up by lectures. This format is considered effective if the intent is solely focused on short-term learning and achieving a course completion certificate, because most providers will pass their test at the end of the course, however evidence shows that after these training courses, skills and knowledge deteriorate after 1 to 6 months.
The spacing effect, the finding that practice distributed over time yields better learning than practice massed more closely together, was first described in cognitive psychology, and was developed at Harvard into a strategy to effectively embed clinical knowledge with more success than any other method.

The ARLS course utilises the principles and practice of adaptive spaced education to both consolidate and assess the vital knowledge taught throughout the course.
A series of 24 focused multiple-choice questions, designed to specifically test the comprehensive ARLS syllabus of resuscitation knowledge, are automatically emailed to candidates following their face-to-face course.
The candidates are invited to answer these, upon which there is immediate feedback on their answer, a description of the evidence underlying both correct and incorrect choices, and links provided for further reading. The questions are re-sent at varying intervals, depending on whether the initial choice was correct or incorrect.
Game theory is employed by showing comparative performance by all candidates in a cohort, This consolidation and assessment takes place over a period of approximately 7-8 weeks.

Once again, similar to ARLS, the PILS course utilises the principles and practice of adaptive spaced education to both consolidate and assess the vital knowledge taught throughout the course.
A series of focused multiple-choice questions, designed to specifically test the PILS syllabus of clinical skills knowledge, are emailed to candidates following their face-to-face course.
The questions are re-sent at varying intervals, depending on whether the initial choice was correct or incorrect; this consolidation and assessment takes place over a period of approximately 4 weeks.

New courses
We are currently heavily involved in the development of new materials and new courses, all of which we plan to be available in 2021, and which will depend on innovative and contemporary educational theory and practice.
Media collaboration
Our new state-of-the art studio facility and our collaboration with media and film professionals, coupled with educational excellence and clinical expertise, will soon deliver learning experiences not previously seen in Australia.

References
Kidd T, Kendall S. Review of effective advanced cardiac life support training using experiential learning. J Clin Nurs 2006; 16: 58–66.
Reed T, Pirotte M, McHugh M, Oh L, Lovett S, Hoyt AE, Quinones D, Adams W, Gruener G, McGaghie WC. Simulation-based mastery learning improves medical student performance and retention of core clinical skills. Simul Healthc 2016; 11: 173–180.
Boysen-Osborn M, Anderson CL, Navarro R, Yanuck J, Strom S, McCoy CE, et al. Flipping the Advanced Cardiac Life Support Classroom with Team-based Learning: Comparison of Cognitive Testing Performance for Medical Students at the University of California, Irvine, United States. JEEHP 2016; 13:11.
Breckwoldt J, Beck S, Beckers SK, Bhanji F, Bigham BL, Bray JE, Cheng A, Duff JP, Gilfoyle E, Hsieh MJ, Iwami T, Lauridsen KG, Lockey AS, Ma M, Monsieurs KG, Okamoto D, Pellegrino JL, Yeung J, Finn J, Greif R. – on behalf of the International Liaison Committee on Resuscitation Task Force Education, implementation and Teams. ‘Pre-course preparation for advanced courses’ Consensus on Science with Treatment Recommendations [Internet] Brussels, Belgium: International Liaison Committee on Resuscitation (ILCOR) Task Force Education, Implementation and Teams, 2020, Jan 3th. Available from: http://ilcor.org
Hunt EA, Duval-Arnould JM, Chime NO, Jones K, Rosen M, Hollingsworth M, Aksamit D, Twilley M, Camacho C, Nogee DP, Jung J, Nelson- McMillan K, Shilkofski N, Perretta JS. Integration of in-hospital cardiac arrest contextual curriculum into a basic life support course: a randomized, controlled simulation study. Resuscitation. 2017; 114: 127–132.
Knight LJ, Gabhart JM, Earnest KS, Leong KM, Anglemyer A, Franzon D. Improving code team performance and survival outcomes: implementation of pediatric resuscitation team training. Crit Care Med 2014; 42: 243– 251.
Meaney PA, Sutton RM, Tsima B, Steenhoff AP, Shilkofski N, Boulet JR, Davis A, Kestler AM, Church KK, Niles DE, Irving SY, Mazhani L, Nadkarni VM. Training hospital providers in basic CPR skills in Botswana: acquisition, retention and impact of novel training techniques. Resuscitation 2012; 83: 1484–1490.
Kerfoot BP. Adaptive Spaced Education Improves Learning Efficiency: A Randomized Controlled Trial. J Urol 2010; 183: 678-681.


